Gastrointestinal (GI) troubles such as nausea, cramps, bloating, diarrhoea and the urge to be sick are common amongst triathletes, particularly during long-course events.
Prior to racing, plenty of triathletes report feeling physically capable of a good race, but later explain that issues with their gut caused them to slow down or withdraw altogether.
The underlying cause of GI problems during exercise is complex and not always attributed to one single factor, but there are a number of nutritional strategies you can try as a means of reducing the likelihood of experiencing symptoms.
One of these strategies is the use of a short-term low FODMAP diet, which was created by researchers in Australia as a means to treat irritable bowel syndrome (IBS).
Since some of the GI symptoms experienced by athletes during exercise are similar to those experienced by IBS patients, the diet has gained popularity as a nutritional strategy amongst athletes who frequently suffer from exercise-induced GI complaints.
What are FODMAPs?
FODMAP stands for fermentable oligosaccharide, disaccharide, monosaccharide and polyols, which are shorter chain carbohydrates that aren’t as efficiently absorbed in the GI tract.
These include foods such as potatoes, wheat, dates and some artificial sweeteners like sorbitol. Their poor absorption means they sit within the GI tract rather than be digested, which can cause water to be drawn into the intestine from the body, leading to diarrhoea and a feeling of fullness.
When they reach the large intestine, FODMAPs are quickly broken down by colonic bacteria, which produces gas and leads to flatulence and bloating.
FODMAP foods
A list of some high-FODMAP foods and their alternatives is shown below:
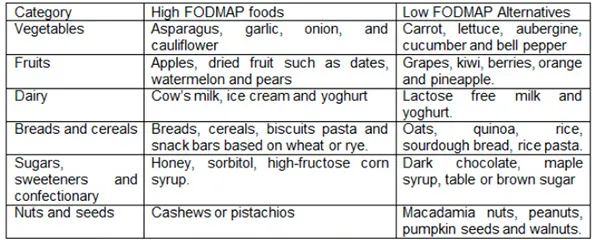
The above table has been adapted from Starting the FODMAP Diet, Monash University.
As you can see, a lot of these foods are recommended as part of a healthy diet and most athletes consume these foods before and during training or competition.
How to get started with FODMAPs
If you’re an athlete struggling with GI problems, then a low-FODMAP diet may be a promising strategy to try. However, there's no one-size fits all approach and the FODMAP diet can be complex, involving the removal of certain foods from the diet for a period of time or from particular parts of your day e.g. pre- or during training.
Removing foods from your diet could lead deficiencies in certain nutrients and, therefore, should always be undertaken under the guidance of a qualified practitioner.
Before committing to a low-FODMAP diet, I'd recommend creating a food diary which also logs your training and occurrence of symptoms, which might help you identify particular ‘trigger’ foods.
You may identify one particular food that's causing issues and a simple switch to an alternative might be all you need. Also consider that it may not be your diet which is causing your GI stress, but perhaps a particular training session such as high-intensity intermittent sprints, or that you may be dehydrated.
References
Costa, R.J.S. Snipe, R.M.J. Kitic, C.M. Gibson, P.R. Systematic review: exercise-induced gastrointestinal syndrome-implications for health and intestinal disease. Aliment Pharmacol Ther. 2017;46(3):246-265
